The Link Between Alcoholism and Depression

Understanding Alcoholism and Depression
To grasp the link between alcoholism and depression, it is important to have a clear understanding of what alcoholism and depression entail. This section will delve into the definitions of alcoholism and depression, as well as shed light on the prevalence of these conditions.
What is Alcoholism?
Alcoholism, also known as alcohol use disorder (AUD), is a chronic condition characterized by an individual's inability to control or stop their alcohol consumption despite negative consequences. It is considered a substance use disorder and can have severe physical, psychological, and social implications.
Alcoholism is typically diagnosed based on criteria outlined in the Diagnostic and Statistical Manual of Mental Disorders (DSM-5). These criteria include factors such as an increased tolerance to alcohol, withdrawal symptoms when alcohol is not consumed, unsuccessful attempts to cut down or control alcohol consumption, and continued alcohol use despite negative consequences.
What is Depression?
Depression, also referred to as major depressive disorder (MDD), is a mood disorder characterized by persistent feelings of sadness, hopelessness, and a loss of interest in activities. It affects how a person thinks, feels, and behaves, often leading to a variety of emotional and physical problems.
Depression can be diagnosed based on the symptoms outlined in the DSM-5. These symptoms may include persistent sadness, feelings of worthlessness or guilt, changes in appetite or weight, difficulty sleeping or excessive sleeping, loss of energy, difficulty concentrating, and recurrent thoughts of death or suicide.
The Prevalence of Alcoholism and Depression
The coexistence of alcoholism and depression is not uncommon. Both conditions have a significant impact on individuals and can exacerbate one another. According to research, the prevalence rates of alcoholism and depression are noteworthy.
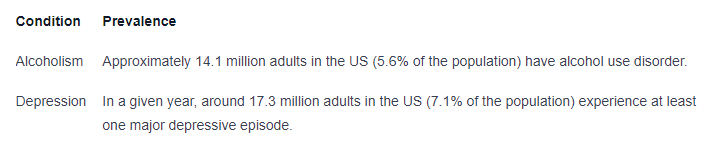
It is important to note that these statistics provide a general understanding of the prevalence of alcoholism and depression, but the actual numbers may vary based on various factors such as age, gender, and geographical location.
By comprehending the definitions of alcoholism and depression, as well as acknowledging their prevalence, we can better explore the intricate relationship between these two conditions and the factors that contribute to their link.
The Relationship Between Alcoholism and Depression
Understanding the relationship between alcoholism and depression is crucial in addressing the challenges faced by individuals dealing with these conditions. This section explores the correlation between alcoholism and depression, the depressant effects of alcohol, and the concept of self-medication and coping mechanisms.
Correlation vs. Causation
When examining the link between alcoholism and depression, it's important to distinguish between correlation and causation. While research has consistently shown a strong association between the two, it does not imply that one condition directly causes the other. Rather, alcoholism and depression often coexist and can exacerbate each other's symptoms.
Alcohol as a Depressant
Alcohol is classified as a depressant, meaning it slows down the central nervous system, leading to relaxation and sedation. While individuals may turn to alcohol as a temporary means of escaping depressive emotions, the long-term effects can worsen symptoms of depression. Alcohol can disrupt the brain's chemistry, affecting neurotransmitters like serotonin, which play a crucial role in regulating mood. This disruption can contribute to the development or intensification of depressive symptoms.
Self-Medication and Coping Mechanisms
Many individuals with depression may turn to alcohol as a form of self-medication, attempting to alleviate their emotional pain or numb their negative feelings. This behavior can provide temporary relief, as alcohol initially produces pleasurable effects by increasing dopamine levels in the brain. However, over time, excessive alcohol consumption can worsen feelings of depression, leading to a vicious cycle of drinking to cope with depressive symptoms.
It's important to note that not all individuals who struggle with alcoholism have depression, and vice versa. However, the risk of developing one condition increases the vulnerability to the other due to the complex interplay of genetic, biological, environmental, and psychological factors.
Understanding the relationship between alcoholism and depression is crucial for effective treatment and support. By recognizing the correlation between these conditions and addressing them holistically, individuals can work towards breaking the cycle and improving their overall well-being. Seeking professional help, utilizing integrated treatment approaches, and building a supportive network are essential steps in breaking free from the grips of alcoholism and managing depression effectively.
Factors Contributing to the Link
The link between alcoholism and depression is influenced by a combination of factors, including genetic and biological factors, environmental and psychological factors, and the presence of co-occurring disorders.
Genetic and Biological Factors
Genetic and biological factors play a role in both alcoholism and depression. Numerous studies have shown that individuals with a family history of alcoholism or depression are at a higher risk of developing these conditions themselves. This suggests a genetic predisposition that can contribute to the link between alcoholism and depression.
Moreover, certain brain chemical imbalances, such as low levels of serotonin and dopamine, have been associated with both alcoholism and depression. These imbalances can impact mood regulation and contribute to the development of both conditions.
Environmental and Psychological Factors
Environmental and psychological factors also contribute to the link between alcoholism and depression. Adverse childhood experiences, such as abuse, neglect, or trauma, can increase the risk of developing both alcoholism and depression later in life. Additionally, chronic stress, social isolation, and poor coping skills can contribute to the development of these conditions.
Furthermore, the presence of other mental health disorders, such as anxiety or post-traumatic stress disorder (PTSD), can increase the likelihood of experiencing both alcoholism and depression. These co-occurring disorders can interact and exacerbate symptoms, making it more challenging to treat and manage these conditions effectively.
Co-Occurring Disorders
The presence of co-occurring disorders, also known as dual diagnosis or comorbidity, is common in individuals with both alcoholism and depression. It is estimated that approximately one-third of individuals with alcohol use disorder also experience depression, and vice versa.
Co-occurring disorders can complicate treatment and recovery efforts as they often interact and influence each other. For example, alcohol use can worsen depressive symptoms, while depression can increase the risk of alcohol relapse. It is essential to address both conditions simultaneously to achieve successful outcomes.
Understanding these contributing factors provides insight into the complex relationship between alcoholism and depression. By considering genetic and biological factors, environmental and psychological factors, and the presence of co-occurring disorders, professionals can develop comprehensive approaches to prevention, early intervention, and treatment for individuals affected by both conditions.
The Cycle of Alcoholism and Depression
Alcoholism and depression often go hand in hand, creating a complex and challenging cycle. Understanding the relationship between these two conditions is essential for effective treatment and support. In this section, we will explore how alcoholism can be a risk factor for depression, how depression can increase the risk of alcoholism, and how these factors contribute to the vicious cycle that individuals may find themselves in.
Alcoholism as a Risk Factor for Depression
Alcoholism can increase the risk of developing depression. Excessive and prolonged alcohol consumption can disrupt the brain's chemistry, affecting neurotransmitters that regulate mood. Additionally, alcohol can have a depressive effect on the central nervous system, exacerbating feelings of sadness and hopelessness.
Alcoholism as a Risk Factor for Depression
Excessive and prolonged alcohol consumption can increase the risk of depression.
Alcohol disrupts brain chemistry and affects mood-regulating neurotransmitters.
Alcohol has a depressive effect on the central nervous system, intensifying negative emotions.
Depression as a Risk Factor for Alcoholism
On the other hand, depression can also increase the risk of developing alcoholism. Individuals experiencing depression may turn to alcohol as a means of self-medication or coping with their emotional pain. Alcohol can temporarily provide a sense of relief and escape, leading to a reliance on alcohol as a way to numb or mask their depressive symptoms.
Depression as a Risk Factor for Alcoholism
Depression can increase the risk of alcoholism as individuals may turn to alcohol as a form of self-medication.
Alcohol temporarily provides relief and escape from depressive symptoms, leading to reliance on alcohol.
Individuals with depression may use alcohol as a way to numb or mask their emotional pain.
The Vicious Cycle
The relationship between alcoholism and depression creates a vicious cycle. Alcoholism can worsen depressive symptoms, leading to a deepening sense of hopelessness and despair. This, in turn, can drive individuals to consume more alcohol as a means of self-medication. The cycle continues as the negative consequences of alcoholism, such as strained relationships, financial difficulties, and health problems, further contribute to feelings of depression.
The Vicious Cycle
Alcoholism worsens depressive symptoms, deepening feelings of hopelessness and despair.
Individuals may consume more alcohol as a form of self-medication.
Negative consequences of alcoholism contribute to feelings of depression, perpetuating the cycle.
Breaking this cycle requires addressing both alcoholism and depression simultaneously. Integrated treatment approaches that focus on both conditions, such as therapy, support groups, and medication, can be effective in helping individuals regain control of their lives and achieve recovery. By understanding the cycle and seeking appropriate help, individuals can find hope and take steps toward a healthier and happier future.
Seeking Help and Treatment Options
When dealing with the complex relationship between alcoholism and depression, seeking professional help and exploring treatment options is crucial. Addressing both conditions simultaneously is essential for effective recovery and improving overall well-being. Here are some common avenues for seeking help and treatment:
Professional Assessment and Diagnosis
To begin the journey towards recovery, it is important to undergo a professional assessment and diagnosis. This typically involves consulting with healthcare professionals who specialize in addiction and mental health. They will evaluate your symptoms, medical history, and personal circumstances to determine the appropriate diagnosis and treatment plan.
During the assessment, healthcare professionals may use various tools and interviews to gather information. They may assess the severity of alcoholism using instruments such as the Alcohol Use Disorders Identification Test (AUDIT) and evaluate depression symptoms using standardized questionnaires like the Beck Depression Inventory (BDI). These assessments help in understanding the extent and impact of both conditions.
Integrated Treatment Approaches
Integrated treatment approaches, also known as dual diagnosis treatment, focus on addressing both alcoholism and depression simultaneously. This comprehensive approach recognizes the interconnected nature of these conditions and aims to provide comprehensive care.
Integrated treatment may include a combination of therapies such as medication, counseling, and behavioral interventions. Medications may be prescribed to manage withdrawal symptoms, reduce alcohol cravings, and alleviate depressive symptoms. Counseling and therapy sessions, such as cognitive-behavioral therapy (CBT) or motivational interviewing, can help individuals develop coping strategies, improve self-esteem, and address underlying issues contributing to both alcoholism and depression.
Support Groups and Therapy
Support groups and therapy can play a vital role in the recovery process. Support groups specifically tailored to individuals with alcoholism and depression can provide a safe and non-judgmental environment for sharing experiences, gaining insights, and receiving encouragement from others who have gone through similar struggles.
Therapy, such as individual therapy or group therapy, offers a structured setting to explore the underlying causes of alcoholism and depression. Therapists can help individuals develop healthier coping mechanisms, improve problem-solving skills, and identify and address triggers that contribute to both conditions.
It is important to note that seeking help is a sign of strength, and no one should face these challenges alone. With the guidance and support of professionals, along with the understanding and encouragement from support groups and therapy, individuals can navigate their way towards recovery and regain control over their lives.
Breaking the Cycle
When it comes to the link between alcoholism and depression, breaking the cycle is crucial for individuals who are struggling with both conditions. By addressing both alcoholism and depression, individuals can take important steps towards recovery and improving their overall well-being. Here are three key aspects to consider in breaking the cycle: recovery and sobriety, managing depression, and building a supportive network.
Recovery and Sobriety
Recovery and sobriety play a central role in breaking the cycle of alcoholism and depression. For individuals with co-occurring alcoholism and depression, it is important to seek professional help and support to overcome alcohol addiction. This may involve participating in rehabilitation programs, attending support groups, or undergoing therapy.
Maintaining sobriety is a continuous process that requires dedication and commitment. It is essential to develop coping mechanisms and healthy strategies to manage triggers and cravings. By actively engaging in recovery programs and adopting a sober lifestyle, individuals can significantly reduce the risk of relapse and create a foundation for a healthier life.
Managing Depression
Managing depression is a vital component of breaking the cycle. It is crucial to address the underlying mental health issues that contribute to both alcoholism and depression. Seeking professional help from therapists or psychiatrists can provide individuals with the necessary tools and strategies to manage their depression effectively.
Treatment options for depression may include psychotherapy, medication, or a combination of both. Cognitive-behavioral therapy (CBT) and other evidence-based therapies can help individuals recognize negative thought patterns, develop healthier coping mechanisms, and improve their overall mood. It is important to work closely with healthcare professionals to find the most suitable treatment approach for managing depression.
Building a Supportive Network
Building a supportive network is essential for individuals who are breaking the cycle of alcoholism and depression. Surrounding oneself with understanding and empathetic individuals can provide the necessary support and encouragement throughout the recovery journey. This network may include family members, friends, support groups, or even online communities.
Having a support system can help individuals stay motivated and accountable. It provides a safe space to share experiences, seek guidance, and receive encouragement. Additionally, support groups specifically tailored for individuals dealing with co-occurring alcoholism and depression can offer valuable insights and a sense of belonging.
By actively engaging in recovery, managing depression, and building a supportive network, individuals can break the cycle of alcoholism and depression. It is important to remember that seeking professional help and support is crucial in this process. With the right resources and a strong commitment to change, individuals can overcome the challenges posed by alcoholism and depression, leading to a healthier and more fulfilling life.
Conclusion
The link between alcoholism and depression is a complex and challenging issue that affects many individuals worldwide. By understanding the contributing factors, such as genetic and biological factors, environmental and psychological factors, and co-occurring disorders, professionals can develop comprehensive approaches to prevention, early intervention, and treatment for individuals affected by both conditions.
Breaking the cycle of alcoholism and depression requires addressing both conditions simultaneously. Integrated treatment approaches that focus on medication, counseling, and behavioral interventions can be effective in helping individuals regain control of their lives and achieve recovery. Additionally, building a supportive network of family members, friends, or support groups can provide the necessary support throughout the recovery journey.
It is important to remember that seeking professional help is crucial in this process. With the right resources and a strong commitment to change, individuals can overcome the challenges posed by alcoholism and depression. By actively engaging in recovery efforts, managing depression symptoms effectively, and building a supportive network of people around them, individuals can break the cycle of alcoholism and depression leading to a healthier life full of fulfillment.
